|
 |
- Search
| J Korean Med Assoc > Volume 48(4); 2005 > Article |
Abstract
Urinary incontinence (UI) is a prevalent condition that can adversely affect a woman's quality of life. The prevalence of UI among Korean women was estimated up to 42% of the married female population. Overactive bladder syndrome (OAB) is a symptomatic diagnosis based on the presence of urgency, with or without urge incontinence, and usually accompanied by frequency and nocturia, in the absence of obvious pathologic or metabolic disease. Stress urinary incontinence (SUI), the complaint of involuntary loss of urine during effort or exertion or during sneezing or coughing, is the most common type of UI among women. Recommended initial evaluation methods of UI include validated symptom-questionnaire, 24 hour-voiding diary, 1-hour pad test, and provocative stress test. The initial management of OAB requires an integrated approach using behavioral and pharmacologic methods. Patients should be educated about the functioning of the lower urinary tract system, fluid and dietary management, timed or prophylactic voiding and bladder training regimens, and pelvic floor exercises (PFE). Although muscarinic receptor antagonists have been shown to be effective for the treatment of OAB, adverse effects, such as dry mouth, constipation, and blurred vision have limited their usefulness. Most cases of OAB are not cured, but the symptoms are reduced, with an associated improvement in the patients' quality of life. Patients who are not benefited by behavioral and pharmacologic intervention may respond to intravesical administration of drugs, including blockers of afferent input; intradetrusor injection of botulinum toxin, neuromodulation, and augmentation cystoplasty. The initial treatment of SUI includes behavioral changes and PFE. Bladder training, vaginal devices, and urethral inserts may also reduce stress incontinence. Surgical procedures are more likely to cure SUI than nonsurgical procedures. Based on a line of evidences available at this time, colposuspension (such as Burch) and pubovaginal sling (including the newer midurethral synthetic slings such as TVT) are the most effective surgical treatments.
References
6. Herzog AR, Fultz NH, Normolle DP, Brock BM, Diokno AC. Methods used to manage urinary incontinence by older adults in the community. J Amer Geriatr Soc 1989;37:339-344.
7. Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Wein A, et al. The standardization of terminology of lower urinary tract function: Report from the standardization subcommitee of international continence society. Neurourol Urodyn 2002;21:167-178.
8. Stamey TA. Endoscopic suspension of the vesical neck for urinary incontinence in females. Report on 203 consecutive patients. Ann Surg 1980;192:465-471.
10. Ulmsten U, Petros P. Intravaginal slingplasty: An ambulatory surgical procedure for treatment of female urinary incontinence. Scand J Urol Nephrol 1995;29:75-82.
11. Blaivas JG, Groutz A. In: Walsh PC, Retik AB, Stamey TA, Vaughan ED, editor. Urinary incontinence: pathophysiology, evaluation, and management overview. Campbell's urology 2002;8th ed. Philadelphia: Saunders. 1027-1052.
12. 1st International Consultation on Incontinence Recommendations of the International Scientific Committee: The evaluation and treatment of urinary incontinence 1998;Incontinence. 945-969.
15. Fantl JA, Wyman JF, McClish DK, Harkins SW, Elswick RK, Hadley EC, et al. Efficacy of bladder training in older women with urinary incontinence. JAMA 1991;265:609-613.
16. Fantl JA. Behavioral intervention for community-dwelling individuals with urinary incontinence. Urology 1998;51:2A Suppl. 30-34.
17. Jackson S. The patient with an overactive bladder? symptoms and quality-of-life issues Urology 1997;50:6A Suppl. 18-22.
18. Andersson KE. 1997, 'The overactive bladder: pharmacologic basis of drug treatment'. Urology 1997;50:6A Suppl. 74-84.
19. Wein AJ. Pharmacologic options for the overactive bladder. Urology 1998;51:2A Suppl. 43-47.
20. Kelleher CJ, Cardozo LD, Khullar V, Salvatore S. 1997, 'A medium-term analysis of the subjective efficacy of treatment for women with detrusor instability and low bladder compliance'. British Journal of Obstetrics and Gynaecology 1997;104:988-993.
21. Drutz HP, Appell RA, Gleason D, Klimberg I, Radomski S. Clinical efficacy and safety of tolterodine compared to oxybutynin and placebo in patients with overactive bladder. International Urogynecology Journal and Pelvic Floor Dysfunction 1999;10:283-289.
22. Appell RA. Electrical stimulation for the treatment of urinary incontinence. Urology 1998;51:2A Suppl. 24-26.
23. Choi JH, Han DH, Cho J, Lee KS. Extracorporeal magnetic stimulation for the treatment of overactive bladder durability of efficacy. Korean J Urol 2003;44:Suppl 2. 160. Abst.
24. Wein AJ. Diagnosis and treatment of the overactive bladder. Urology 2003;62:20-27.
25. Macdiamind SA. Overactive bladder: Improving the efficacy of anticholinergics by dose escalation. Curr Urol Rep 2003;4:446-451.
26. Andersson KE, Yoshida M. Antimuscarinics and the overactive detrusor-which is the main mechanism of action? Eur Urol 2003;43:1-5.
27. Hohenfellner M, Dahms SE, Matzel K, Thuroff JW. Sacral neuromodulation for treatment of lower urinary tract dysfunction. BJU Int 2000;85:Suppl 3. 10-19.
28. Wein AJ. In: Walsh PC, Retik AB, Vaughan ED, et al, editor. Neuromuscular dysfunction of the lower urinary tract and its management. Campbell's Urology 2002;8th ed. Philadelphia: WB Saunders Co.. 931-1026.
29. Payne CK. In: Walsh PC, Retik AB, Vaughan ED, et al, editor. Urinary incontinence: nonsurgical management. Campbell's Urology 2002;8th ed. Philadelphia: WB Saunders Co.. 1069-1091.
30. Lee KS, Chung KJ, Kim JC, Joo MS. The effect of sacral neuromodulation in patients with the interstitial cystitis resistant to conservative treatment. Korean J Urol 2003;44:Suppl 2. 74. Abst.
31. Schurch B, Stohrer M, Kramer G, Schmid DM, Gaul G, Hauri D. Botulinum-A toxin for treating detrusor hyperreflexia in spinal cord injured patients: a new alternative to anticholinergic drug? Preliminary results J Urol 2000;164:692-697.
32. Gross M, Boone TB, Appell RA. Surgical management of overactive bladder. Curr Urol Rep 2002;3:388-395.
33. Westney OL, Lee JT, McGuire EJ, Palmer JL, Cespedes RD, Amundsen CL. Long-term results of Ingelman-Sundberg denervation procedure for urge incontinence refractory to medical therapy. J Urol 2002;09. 168:1044-1047.
34. Chanceller MB. New frontiers in the treatment of overactive bladder and incontinence. Rev Urol 2002;4:S50-S56.
35. Atala A. Tissue engineering for the replacement of organ function in the genitourinary system. Am J Transplant 2004;4:Suppl 6. 58-73.
36. Cardozo L, Bachmann G, McClish D, Fonda D, Birgerson L. Meta-analysis of estrogen therapy in the management of urogenital atrophy in postmenopausal women: second report of the Hormones and urogenital Therapy committee. Obstet Gynecol 1998;92:722-727.
37. Kegel A. Progressive resistance exercise in the functional restoration of the perineal muscles. Am J Obstet Gynecol 1948;56:238-248.
39. Bo K, Talseth T. Long-term effect of pelvic floor muscle exercise 5 years after cessation of organized training. Obstet Gynecol 1996;87:261-265.
40. O'Donnell PD, Doyle R. Biofeedback therapy technique for treatment of urinary incontinence. Urology 1991;37:432-436.
41. Kralj B. In: Ostergard DR, Bent AE, editor. The treatment of femalle urinary incontinence by functional electrical stimulation. Urogynecology and Urodynamics Theory and Practice 1996;4th ed. Baltmore: Williams & Wilkins. 555.
42. Ericksen BC, Eik-Nes SH. Long-term electrostimulation of the pelvic floor: primary therapy in female urinary incontinence? Urol Int 1989;44:90-95.
45. Enzelsberger H, Helmer H, Schatten C. Comparison of Burch and lyodura sling procedures for repair of unsuccessful incontinence surgery. Obstet Gynecol 1996;88:251-256.
46. Lalos O, Berglund AL, Bjerle P. Urodynamics in women with stress incontinence before and after surgery. Eur J Obstet Gynecol Reprod Biol 1993;48:197-205.
47. Ulmsten U, Falconer C, Johnson P, Jomaa M, Lanner L, Olsson I, et al. A multicenter study of tension-free vaginal tape (TVT) for surgical treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 1998;9:210-213.
48. Ulmsten U, Johnson P, Rezapour M. A three-year follow up of tension free vaginal tape for surgical treatment of female stress urinary incontinence. Br J Obstet Gynecol 1999;106:345-350.
49. Meschia M, Pifarotti P, Bernasconi F, Guercio E, Maffiolini M, Spreafico L, et al. Tension-free vaginal tape: analysis of outcomes and complications in 404 stress incontinent women. Int Urogynecol J 2001;12:Suppl 2. S24-S27.
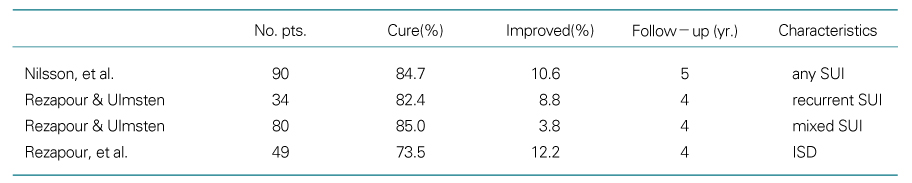
50. Nilsson CG, Kuuva N, Falconer C, Rezapour M, Ulmsten U. Long-term results of the tension-free vaginal tape(TVT) procedure for surgical treatment of female stress urinary incontinence. Int Urogynecol J 2001;12:Suppl 2. S5-S8.
51. Rezapour M, Ulmsten U. Tension-free vaginal tape(TVT) in women with recurent stress urinary incontinence-A longterm follow-up. Int Urogynecol J 2001a;12:Suppl 2. S9-S11.
52. Rezapour M, Falconer C, Ulmsten U. Tension-free vaginal tape(TVT) in stress incontinent women with intrinsic sphincter deficiency(ISD)-A long-term follow-up. Int Urogynecol J Pelvic Floor Dysfunct 2001;12:Suppl 2. S12-S14.
53. Nilsson CGN, Rezapour M, Falconer C. 7 years follow-up of the tension-free vaginal tape procedure. Annual IUGA Meeting Abstract 2003;14:S35.
54. Ward KL, Hilton P. UK and Ireland TVT Trial Group. A prospective multicenter randomized trial of tension-free vaginal tape and colposuspension for primary urodynamic stress urinary incontinence: Two-year follw-up. Am J Obstet Gynecol 2004;190:324-331.
55. Deval B, Levardon M, Samain E, Rafii A, Cortesse A, Amarenco G, et al. A French multicenter clinical trial of SPARC for stress urinary incontinence. Eur Urol 2003;44:254-258.
56. Balmforth J, Cardozo LD. Trends toward less invasive treatment of female stress urinary incontinence. Urology 2003;62:Suppl 4A. 52-60.
57. Boustead GB. The tension-free vaginal tape for treating female stress urinary incontinence. BJU Int 2002;89:687-693.
58. Hardart A, Klutke JJ, Klutke CG, Carlin B. Altered voiding after the tension-free vaginal tape procedure. Is increased resistance the mechanism of therapy. Obstet Gynecol 2000;95:Suppl 1. S35.
- TOOLS
-
METRICS

-
- 3 Crossref
- Scopus
- 1,161 View
- 8 Download
-
Related articles in
J Korean Med Assoc -
Diagnosis and treatment of dyslipidemia in children and adolescents2024 May;67(5)
Diagnosis and treatment of dysphagia2023 October;66(10)
Diagnosis and pharmacological management of allergic conjunctivitis2023 September;66(9)
Diagnosis and treatment of adult spinal deformity2023 August;66(8)
Diagnosis and treatment of patellofemoral joint arthritis2023 August;66(8)